Approximately 7 Minutes Reading Time
Brief Article Overview
- Running is a fantastic form of exercise, with a low barrier of entry.
- Unfortunately, chronic pain is commonly associated with running.
- Modern pain science has repeatedly shown that the state of tissues (muscles, tendons, bone) is not strongly linked with pain, especially over prolonged periods of time.
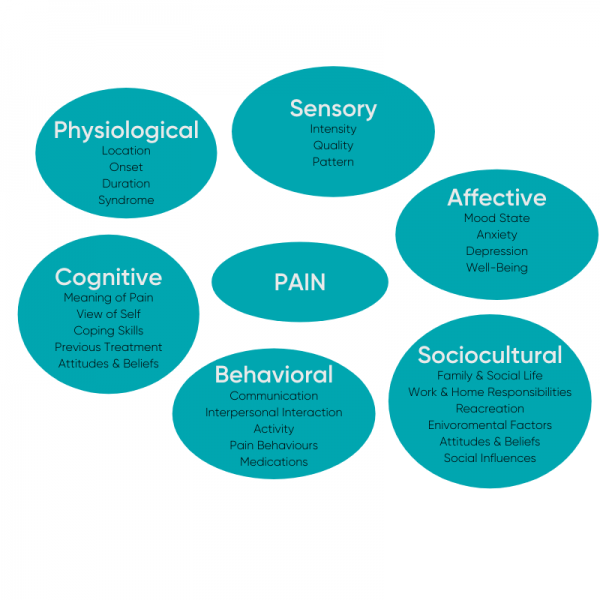
- The state of tissues (bio), your emotional state (psycho), your immediate environment and social support (social) all contribute to the pain problem.
- This is known as the “Biopsychosocial Model”.
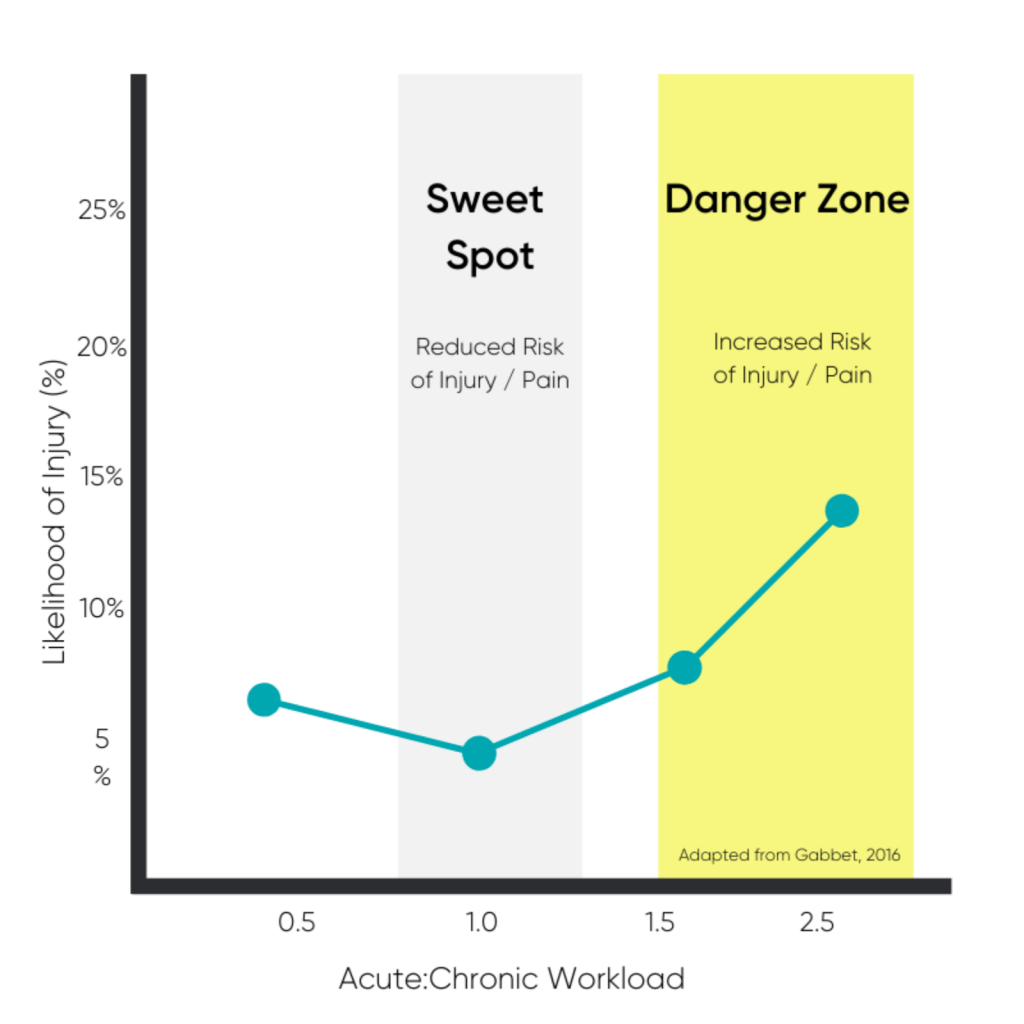
- Usually, pain occurs simply because of doing too much, too soon. So being more strategic with training volume would be the first port of call.
- As well as figuring out the physiological/mechanical causes, we suggest incorporating emotional and social factors as possible influencers for chronic pain too.
Introduction
Who doesn’t want to feel the famous runners high? That state of euphoria experienced after a good run. We love working with endurance athletes. There are plenty of events throughout the year that provide a clear and objective goal to aim for, giving a strong sense of focus and direction.
Sadly, there is also a high incidence of chronic pain associated with long-distance running. Knees, hips, lower back, shins, feet…the list goes on! One UK study reported a 50% injury rate amongst recreational runners, with 86% of those continuing to run through the pain!
Eventually, this pain can act as a barrier to exercise and something as simple as going out for a park run can seem like a struggle. This can be pretty frustrating, especially if you’re training for a specific event. The ability to accumulate training volume (going longer and faster) is the name of the game! The aim of this article is to touch a little on modern pain science to develop a strategy that will help your resolve the problem of training through pain.
 Common Purpose Team
Common Purpose Team