Approximately 8 Minutes Reading Time
Brief Article Overview
- Nutrition is important for good health, which is especially important during pregnancy.
- Nutrition guidance can be confusing and it’s difficult to know what to prioritise when it comes to eating to support pregnancy.
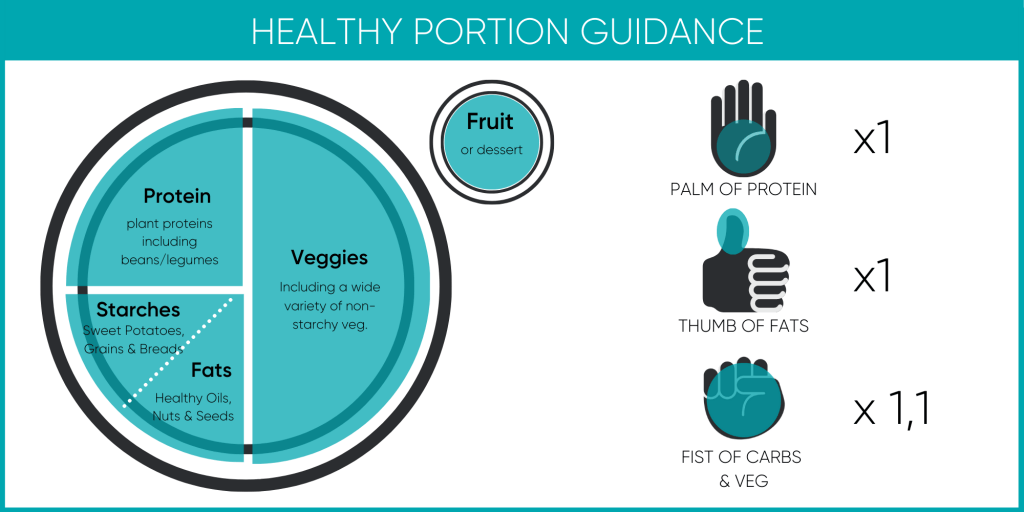
- Before worrying about counting calories, we find that building healthy eating habits, monitoring portions and eating mindfully are the foundations of any good nutritional strategy.
- In general, calorie intake will increase throughout the pregnancy to provide the extra energy needed for the baby to grow and for you to carry it.
- There are certain foods and eating behaviours that may contribute to heartburn and morning sickness.
- There are also certain foods and chemicals which should be limited or avoided altogether.
- Specific supplement advice should be given by a medical professional off the back of a full medical history and blood tests, however, there are supplements that are commonly recommended specifically to support pregnancy.
Introduction
Trying to master healthy eating practices can be difficult at the best of times. It feels like there are new studies being published almost every day that offer conflicting guidance to the diets we once thought were healthy. Trying to understand what a healthy diet is when you’re pregnant can be even more confusing. It’s likely that you’ll become more focused on eating healthily and, perhaps, start to do your own research in regards to eating specifically for pregnancy.
You’ll hear and read conflicting (and often misleading) advice about what to eat. This might include things like “you should be eating X more calories” or “you need to be eating for two”. We hope the information in this article helps guide you through this topic and gives you a full and comprehensive picture of what eating healthily looks like and general recommendations for supporting a healthy pregnancy.
Healthy Habits vs Calories
We recommend you focus on practising basic foundational eating habits rather than counting calories. This may seem a little contradictory since it’s relatively common knowledge that pregnancy requires more calories (and more nutrients) during trimester two, three and whilst breastfeeding. Counting calories isn’t an exact science and there can often be a significant disparity in the calories your body utilises, as well as the reported calorie content on the packet (which can carry up to a 25% error rate).
Setting daily calorie targets can provide additional stress for some, which may be counterproductive as the body probably doesn’t need more stress throughout pregnancy. Getting the required calories and nutrients is easy enough when practising healthy portion control within a varied diet and eating mindfully.